This article was medically reviewed by Dr. Sukrut Dwivedi.
Is the COVID-19 virus mutating? The answer is, yes. However, what does this mean for public health and the pandemic moving forward?
In this blog, ID Care infectious disease specialist, Dr. Sukrut Dwivedi answers some of the many questions people are asking when it comes to COVID-19 mutations such as: What causes viral mutations? How are SARS-CoV-2 mutations occurring? Will these mutations have an impact on the pandemic and the effectiveness of the vaccine?
What Causes Viruses to Mutate?
Viral mutations might sound scary, but the truth of the matter is that viruses mutate; it’s what they do. “When viruses replicate over and over again, occasionally small errors occur, similar to when you’re typing and typos occur,” said Dr. Dwivedi. “So, when viruses get these small errors, those are what we call mutations.”
In the case of COVID-19, should mutations be a cause of concern?
“A lot of time, mutations don’t have much clinical significance,” said Dr. Dwivedi. “Either mutations don’t affect the function of the virus at all, or sometimes mutations can actually work in a negative aspect for the virus, rendering them less harmful. However, sometimes when a virus mutates, it’s beneficial to the virus, allowing it to spread into a new strain, continuing the infectious process. And this seems to be the case with COVID-19.”
So, how is COVID-19 mutating, and what potential does it have for furthering the life of the virus?
SARS-CoV-2 Variants: Three Strains
As of the writing of this blog post, there are three new strains of COVID-19 that have been attracting attention across the United States.
United Kingdom strain (B.1.1.7): This SARS-CoV-2 variant was first detected in the US at the end of 2020. As of today, it has been readily identified across multiple states.
South African strain (B.1.351): Originally detected in early October of 2020 in South Africa, the South African strain shares many similarities with the United Kingdom strain. The first reported cases of the South African strain in the US arose recently at the end of January 2021 in South Carolina.
Brazilian strain (P.1):This SARS-CoV-2 variant was first identified in travelers from Brazil, who were tested during routine screening at an airport in Japan, in early January 2021. This variant was first detected in the US, in the state of Minnesota, at the end of January 2021.
California strain (B.1.427/429): Discovered in early February in Southern California, this variant presents higher transmissibility and increased antibody resistance, similar to the United Kingdom, South African, and Brazilian strains.
New York strain (B.1.526): Recently identified in New York City and surrounding areas, this variant may reduce the ability of certain antibodies to neutralize, or inactivate, the virus, and may help the coronavirus partially evade COVID-19 vaccines.
According to Dr. Dwivedi, through initial observations, the three SARS-CoV-2 mutations do seem to be a bit different from one another. “The United Kingdom strain is thought to be a bit more transmissible, so obviously that’s a concern because it’s more likely to spread amongst individuals. With the South African strain, there’s some indication that the medications or the vaccines we utilize may not necessarily be as effective on this variant. And lastly, the Brazilian strain is also of concern because there seems to be a higher possibility of re-infection after having recovered from COVID-19.”
So, what do the threes strains mean for the state of the pandemic moving forward?
How the New COVID-19 Variants Will Impact the Pandemic
All three of these strains seem to spread more easily and quickly than other variants. However, more research is needed to understand how widely these new variants have spread, how the disease caused by these new variants differs from the disease caused by other variants that are currently circulating, and how these variants may affect existing therapies, vaccines, and tests.
As of the writing of this blog post – according to data collected by The COVID Tracking Project – the US has recorded its lowest number of new daily COVID-19 cases since October 2020, with a majority of states seeing hospitalization rates dropping by 10% or more over the last week. However, despite the promising recent figures, the US is far from out of the woods due to the accelerating spread of virus variants such as the United Kingdom, South African, and Brazilian strains. In fact, nearly 700 cases associated with coronavirus mutations have been identified in the United States, with 690 of those cases being the more easily transmissible United Kingdom strains.
While information about the new strains is constantly emerging, it is fairly obvious that moving forward the new strains are going to impact the pandemic in a couple of different ways. “I believe the United Kingdom strain is most likely going to become the more prevalent strain over the next couple of weeks to two months,” said Dr. Dwivedi. “If that does occur, we know that that the strain is more efficient and rapid in terms of transmission. Obviously, that’s going to increase the number of cases, and unfortunately as the number of cases increase, that will correlate with the number of individuals that are going to end up getting hospitalized. And obviously, the increase in the number of cases will put more strain on health care resources, and potentially lead to more deaths.”
Will the New SARS-CoV-2 Mutations Be Able to Infect Those Who have Already Received the COVID-19 Vaccine?
“That’s definitely a big concern,” said Dr. Dwivedi. “The COVID-19 vaccines are designed to make neutralizing antibodies, and what we’re seeing in laboratory studies is that some of these strains, especially the South African variant, have the ability to decrease the potency of neutralizing antibodies. However, while we know the South African strain has the ability to decrease the potency of neutralizing antibodies, we don’t know if that decrease will be enough to be clinically relevant. So, it’s something to keep an eye on.”
While these new variants may cause some immediate alarm, scientists and researchers are hard at work in finding answers to overcoming the impact of these new strains. But thankfully, the greatest tool we have for combatting the COVID-19 variants is already in process, and it has been since the end of last year.
The COVID-19 Vaccination Roll Out, Herd Immunity, and Improving Vaccines
As of the writing of this blog post, only 2.9 percent of the US population has received a vaccination. And while this number might feel low, many of the individuals who have received their immunizations are seniors living within long-term care facilities – and the numbers are promising.
According to data from the US Centers for Medicare and Medicaid Services, vaccinations have been credited with driving a 50% decrease in infections within nursing homes in the span of four weeks. This means the vaccinations are working, and they will continue to become even more effective as time moves on. “If a virus is going to mutate, we can’t stop it,” said Dr. Dwivedi. “However, what we can do is stop the replication of viruses by decreasing the number of individuals that get infected. And that’s why vaccinations are so important. The more individuals we vaccinate, the less likely it is that these individuals are going to get infected, which ultimately means less chances the virus will have to mutate.”
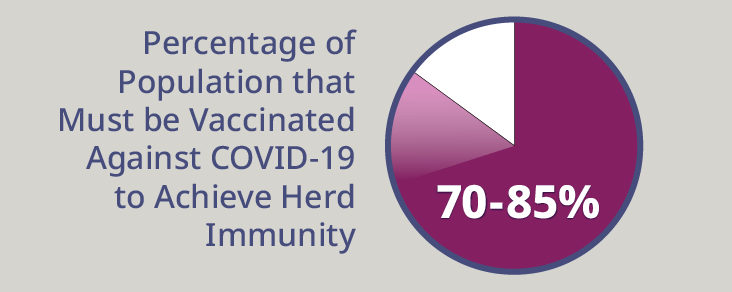
Herd immunity remains the most promising way to stop the spread of COVID-19. The general population is moving closer to that 70-85% threshold of immunity every day; that is still the best defense for decreasing the emergence of variant strains and ending this pandemic once and for all. However, all that being said, shouldn’t scientists be working on a more targeted way to stop the impact of the United Kingdom, South African, and Brazilian variants?
“Yes,” said Dr. Dwivedi. “And they are. Scientists are hard at work improving the vaccines we already have to better handle these new strains. In fact, many companies, like Moderna and Pfizer, have been able to identify the way these newer strains are able to negate the effectiveness of the vaccines. So, they’ve returned to the lab and are working on boosters to ensure the vaccines are as effective as possible.”
Despite the emergence of these new variants, there is light at the end of the tunnel, and Dr. Dwivedi is hopeful about the vaccination process thus far. “It is encouraging that the demand for the vaccine is very high. A lot of individuals I talk to – either at ID Care or in my daily life – have a similar complaint. They’re trying to get the vaccine, but they can’t. And I understand that must be discouraging for them, to have to wait, but for me, an infectious disease specialist, it’s very encouraging. It means that people are very excited and willing to get the vaccine, so much so that the demand is outpacing the supply. So, my advice to everyone is to be patient, as every day the vaccine is being administered, we’re building herd immunity as a population and we’re becoming stronger as a population. And I think if we can continue to improve the process along the way, improve the lines of communication, we will get through this together.”
Conclusion
Keep in mind, while scientists and researchers are working to ensure the public remains safe from these variants, we all must continue to do our part in limiting the spread of COVID-19. If you are feeling anxious about the new variants there are many ways to protect yourself and others. As stated earlier, first and foremost, schedule a vaccination. But also remember to continue physical distancing, use masks, wash your hands, and quarantine when feeling ill.
As the largest independent infectious disease practice on the East Coast, ID Care is always up to date on the latest information concerning COVID-19 variants as well as mitigation strategies patients and healthcare organizations can use to stop the spread of COVID-19. To learn more, visit idcarestg.wpengine.com or call 908-281-0610 to schedule a consultation with an ID Care expert.